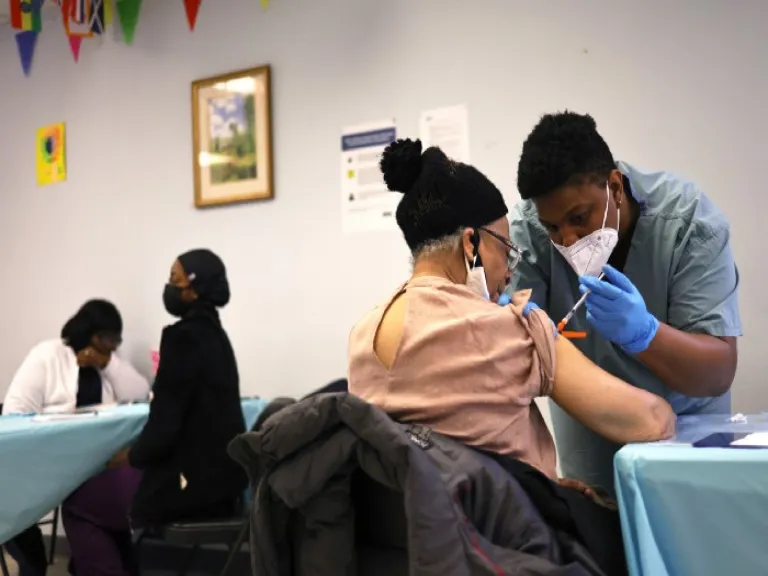
What’s Driving Inequitable Covid-19 Vaccine Distribution?
Covid-19 vaccines emerged as a medical breakthrough, but like many other innovations, they have been disproportionately helping white Americans as compared to other racial and ethnic groups.
As of February 2021, a stark Covid-19 vaccine disparity remains. In Delaware, Black people account for 24% of statewide Covid-19 cases, yet only 9% have received the vaccine. Similarly in Colorado, Hispanic people account for 36% of Covid-19 cases, but only 6% have been vaccinated.
“I’ve heard from [Black and Latino] patients that they want the vaccine, but there is a supply issue and that will continue to be an issue over the next few months.”
There has been a lot of discussion about vaccine hesitancy in Black and Latino communities rooted in a history of medical racism in those communities. However, vaccine skepticism is not the main factor fueling these massive disparities in vaccination.
“Even some of those who want to get the vaccine in disadvantaged communities have not been able to do so,” explains Ryan Neal, MD, Division Head of Hospital Medicine at Houston Methodist in Texas. “I’ve heard from [Black and Latino] patients that they want the vaccine, but there is a supply issue and that will continue to be an issue over the next few months.”
A myriad of systematic and social factors, rooted in racial and socioeconomic inequities, has led to the lack of vaccines in the communities that need them the most.
Improper handling of vaccine distribution
“I think the states and local municipalities were dealt a really bad hand and tried to distribute vaccines initially without appropriate funding or logistical support from the federal government. The good news is that this appears to be improving,” says Laolu Fayanju, MD, senior medical director at Oak Street Health in Ohio.
The scarcity of available vaccines stemming from improper handling of vaccine distribution has exacerbated many of the health disparities driving the vaccine inequities.
“In a space of scarcity the worst instincts come out, and the worst aspects of a social environment that is racist, classist, sexist, and capitalist comes to the surface. It produces and then reinforces existing inequity,” says Chidinma Ibe, PhD, assistant professor at Johns Hopkins School of Medicine.
What’s more, many vaccines are being distributed to national grocery stores and pharmacies such as Kroger, Walgreens, and CVS. According to Fayanju, these national chains do not exist in the kind of working-class but underserved neighborhoods that many of his patients reside in.
“We’re putting vaccines in communities where access is not an issue and we’re not putting vaccines in places where it has been harder historically to get care,” he says.
In addition, the assigning of vaccines to urgent care centers over preventative care centers drove some of the inequities in New York’s vaccine distribution efforts, says Ramon Tallaj, MD, chairman of the board of SOMOS community care, a physician-led health care provider network for New York Medicaid beneficiaries.
“Preventative care is done in the community by doctors. In some places we have a million patients,” Tallaj says. “ If they had given vaccine doses to [preventative care doctors], we would have distributed it to our [underserved] patients knowing the age and the group.”
Lack of community collaboration in distribution planning
Initial vaccine distribution plans failed to properly integrate community leaders and members into planning policies.
“I think it’s interesting that we always ask the experts for input on why disadvantaged communities are hesitant to get the vaccine. One of the things that has bothered me is that I don’t think we’ve heard strongly from the voices of patients who are awaiting vaccines,” Neal adds.
“The leaders who have done a really good job of centering equity in vaccine distribution have been those who were willing to engage with community partners, with people who are on the ground and have lived experiences in the neighborhoods who have been hardest hit by the coronavirus,” says Ibe.
Reverend Barbara Felker, Northwell Health’s VP of strategic community partnerships, also believes that community engagement is critical to success. “The pastors and the community-based organizations know how to do outreach,” she says. And most importantly, the faith-based organizations and faith-based leaders are the trusted entities of the community.
Widespread digital disparities
“In a number of states, it is a chaotic distribution situation, so there’s not an orderly way of signing up for vaccinations,” says Joshua Sharfstein, MD, professor at Johns Hopkins School of Public Health.
The lack of a standard sign-up process means people have to hunt for how to register, which can be a time-intensive task. On top of that, nearly all these sign-ups are online. This makes registering for a vaccine inconvenient, if not impossible, for a sizable portion of Americans.
“This disadvantages low-income communities of color, where many people may not have the time or computer access to monitor multiple websites for hours at a time to spot when openings appear,” Sharfstein says.
10% of the general American population does not have internet access. However, the rate for internet inaccessibility jumps to 27% for older Americans, 15% for Black Americans, 14% for Hispanic Americans, and 18% for Americans with an annual income under $30,000 a year.
Fayanju suggests bridging the digital divide, a disparity that affects vaccine sign-ups.
“The low-tech methods of reaching people help. Shoe-leather solutions that include phone calls, community health workers making direct outreach to people, and a door-to-door, neighborhood-to-neighborhood strategy.”
All is not lost
Different organizations around the country are working to give communities of color an equal chance at a vaccine.
“We distributed vaccines in the public housing community rooms to increase access to vaccines and eliminate the need to travel to another location,” says Felker. She adds, “We have partnered with faith-based leaders to give testing and vaccines out at their church so that seniors and those with physical disabilities are not required to travel to a stadium or an arena, which may not be near their community.”
Neal’s hospital, Houston Methodist, has worked to offer no-cost rides to patients to get vaccines to help bridge the transportation disparity that could prevent patients from having access to vaccination.
These approaches will help. But to truly create health equity, we need to reanalyze the ways we distribute health care and make health equity a core focus of any health care mandates.
The approaches will help. But to achieve deep and lasting health equity, we must move past platitudes and promises for reform and confront the factors that continue to let inequality thrive. Health equity must be the focal point of all future health care initiatives to truly give communities of color the same access to living healthy and vital lives as everyone else.
https://adulted.instructure.com/eportfolios/471/Home/____2021___TWHDBLURAY
https://adulted.instructure.com/eportfolios/473/Home/100___100WOLF_2021100_1080P
https://adulted.instructure.com/eportfolios/473/Home/HD__100__100WOLF__2021_Chinese_HD
https://adulted.instructure.com/eportfolios/474/Home/100____2021__100_TWHDBLURAY
https://adulted.instructure.com/eportfolios/474/Home/100____2021_100WOLF___4K

- The Tokyo Olympics organizing committee fired the director of the opening ceremony on Thursday over a joke he made about

- Can home-schooled youngsters must exact very same techniques as individuals in Cincinnati Universities? You could find a

- Sega forces Yakuza: Like a Dragon off of SteamDB over piracy fears A DMCA takedown notice was sent to SteamDB’s hosting service

- The whole point of certification is that it independently and impartially verifies that you are complying to a standard. Irrespective of regardless